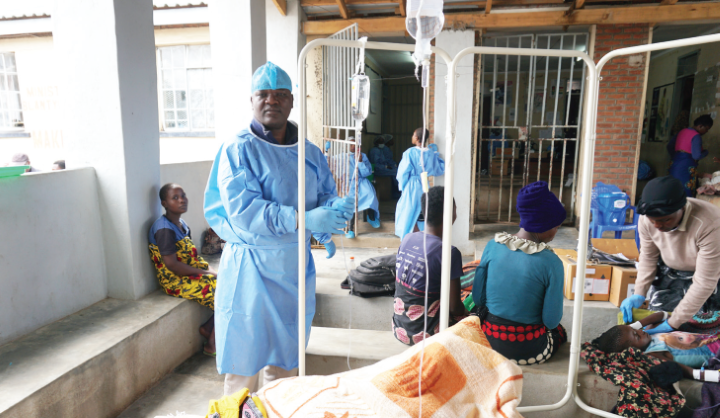
Central hospitals heading for disaster with drug shortage
Drug shortage and lack of district hospitals in the country’s cities has overstretched the health system, paralysing delivery of proper health services in central hospitals.
Malawi’s health care delivery system is divided in three levels, namely, primary, secondary and tertiary. They are linked to each other through an elaborate referral system.
The central hospitals, which fall under tertiary level, are: Mzuzu Central Hospital, Kamuzu Central Hospital, Zomba Central Hospital and Queen Elizabeth Central Hospital.
“These hospitals provide specialist referral health care for their respective regions. Specialist hospitals offer very specific services such as obstetrics and gynaecology,” says Ministry of Health spokesperson Henry Chimbali.
Primary level care consists of community initiatives, health posts, dispensaries, maternity wings, health centres and community and rural hospitals.
“Services at this level are conducted through door-to-door visitations, village clinics, mobile clinics or health posts,” says Chimbali
Services offered include: HIV testing and counselling, immunisation, community case management of acute respiratory infections, diarrhoea, pneumonia and other diseases common to children under the age of five.
The secondary level category consists of districts hospital which handle referral cases from facilities such as health centres and rural or community hospitals. They service local town population, offering both in and out-patient services. Christian Health Association of Malawi (Cham) hospitals also fall under this category.
So if, for instance, a patient at Gola Health Centre in Chikhwawa is referred to Chikhwawa District Hospital and still does not get the expected treatment, the patient has to be referred to a facility such as Queen Elizabeth Central Hospital (QECH) in Blantyre where he or she can get specialised treatment.
However, it has been discovered that the referral system is under threat as some patients choose to use short cuts. This is more pronounced now when the health sector is in a crisis due to acute shortages of drugs and equipment in the public hospitals.
The lower level hospices are struggling even harder because they continually run out of medical kits. As a result, patients and guardians somehow refer themselves to upper level hospitals.
Now, more patients are by-passing the primary and secondary level hospitals, hoping it is in central hospitals where they can get the care they need.
But when they get there, they are usually surprised to see that they cannot even get a basic painkiller.
“I went to Kamuzu Central Hospital and was asked to buy Panado from a private pharmacy because the hospital did not have the drug,” said one patient.
Yet, people continue flocking the central hospitals with ailments, some of which are minor such as wound dressing or a mere headache.
“People are no longer following the referral procedure. They come straight from a health centre to the central hospital,” admitted Dr.Titha Dzowela, deputy director of clinical services in the Ministry of Health.
This puts pressure on resources at central hospitals such as Zomba where the only doctor is working as an administrator and those working in the wards are volunteer doctors.
“The hospital has no Malawian doctors in the wards,” confirmed the hospital director Dr. Martias Joshua.
Zomba Central Hospital has between 600 and 700 in-patients and about 700 out-patients a day. The majority come from Mangochi, a district located several kilometres away.
Chimbali says there are more by-passers in cities that have no district hospitals.
“These are Zomba, Blantyre and Lilongwe,” he said, adding that the Ministry plans to construct district hospitals and strengthen the surrounding urban health centres.
Mzuzu is another central hospital hit by understaffing and is under resourced, yet continues to be overcrowded as people prefer it to their respective health centres or district hospital.
Thanks to United Nations volunteer doctors such as specialist physician Sefu Uledi, the burden is slowly easing. He said there is need to strengthen district hospitals and health centres.
“Imagine doctors at a central hospital are busy with small cases like tooth extraction instead of dealing with critical referral cases. This is a waste of time and resources,” says Uledi.
But with a deteriorating health service delivery system in the country, the fix seems to be here to stay.
“When asked why they did not go to health facilities closer to their homes, they complain of lack of drugs and equipment or that the health worker is not there to give them treatment,” adds Dr. Uledi
What this situation means is that the central hospitals have to brace for tough times ahead.
Dr Kabeya Biselele, a volunteer specialist at Zomba Central, says it does not make sense that the majority of patients that go to the hospital are from Mangochi, yet the district has its own district hospital.
“There is critical over-crowding and we have a critical shortage of staff. As a result, the staff always has an over-loaded schedule and short supply of equipment and other necessities,” Biselele says.
Chimbali admits the pressure that central hospitals have.
“When people by-pass health centres, the pressure is not only on human resources, but also on drugs and other resources to manage ailments,” he says.