Deadly, expensive, preventable
Triumph over polio calls for more funding for vital vaccines, our Features Editor JAMES CHAVULA writes.
Charles George was born a year before Malawi kicked out polio 25 years ago.
But the 26-year-old was not as lucky: he lost a left leg to the contagious virus.
“Since doctors amputated my left leg in 1991, I could not go places and play with friends. I even dropped out of school in Standard Seven,” he says.
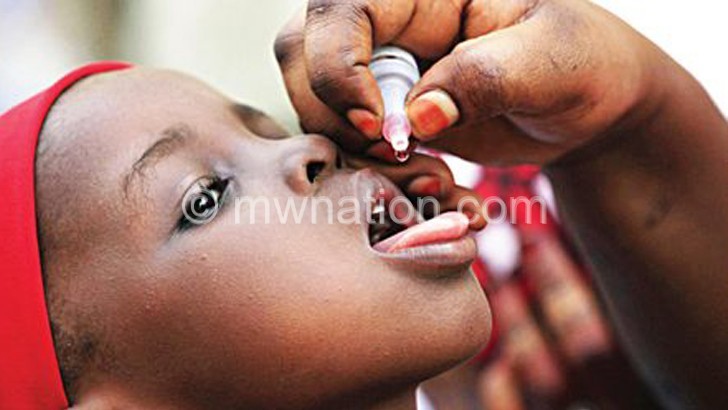
Then, polio was paralysing more than 350 000 children each year globally.
Cycling for a living a kilometre at a time, George personifies triumph over this adversity.
He uses a single leg to peddle a bicycle taxi.
It carries people and goods up and down the steep slopes in the tea-growing town of Luchenza for a fee.
He has one plea: Government must ensure no baby is exposed to the vaccine-preventable infection that robbed him of the leg in his babyhood.
“Polio crushed my dreams. It has almost been eliminated through immunisation, but we must do everything to stop the return of the disease which erodes children’s health and chances in life,” he says.
$44 gain
According to World Health Organisation (WHO) regional director for Africa Dr Matshidiso Moeti, vaccinated children are more likely to stay in school and ultimately enrich the economy.
“Every dollar spent on childhood vaccinations yields $44 [about K33 000] in economic benefits,” she said.
However, Malawi is among African countries that need to accelerate their efforts to reap the dividends that come with investing in child health.
The country’s national immunisation coverage rate—measured by percentage of children receiving the polio vaccine and third dose of the diphtheria-tetanus-pertussis vaccine—dropped from 91percent in 2014 to 84 percent in 2016.
This is below the Global Vaccine Action Plan (GVAP) target of at least 90 percent coverage.
However, Ministry of Health spokesperson Adrian Chikumbe says the country’s immunisation is on track.
“In Malawi, our immunisation coverage is well above WHO targets. This is why the country still gets funding from the Global Alliance for Vaccines [Gavi],” he says.
Despite fears of the recurrence of polio, Chikumbe is optimistic the virus was kicked out for good.
He explains: “Malawi last diagnosed a case of polio in 1992, but we are on a high alert and continue to vaccinate children against the disease because some countries still have a wild virus in circulation.
“Recent reports of new polio cases turned out to be acute flaccid paralysis and tests show it is not caused by polio virus.”
Malawi high-alert response to prevent the resurgence of polio remains a fragile fight against a familiar public health threat as the national immunisation programme is highly donor-dependent.
In fact, only 11 countries in Africa fund more than half of their immunisation programmes.
New challenge
Today, WHO, Gavi and US Agency for International Development (USAid) are expected to announce decisive funding shifts at a meeting to be graced by Regional Immunisation Technical Advisory Group (RTAG) chairperson Professor Helen Rees.
According to Global Health Strategies manager Narmeen Haider, the RTAG meeting is particularly timely as Africa is about to face several funding transitions that will make domestic investments in immunisation more critical than ever.
Warns the health strategist: “As Africa nears polio eradication, critical funding for immunisation through the polio eradication programme is expected to decrease. Additionally, countries approaching middle-income status will transition away from Gavi support for immunisation in the coming years.”
Malawi will need to increase investments in immunisation urgently to ensure that hard-fought gains are not reversed, she says.
The historic promise
Increasing vaccine-related funding is part of the requirements of the Ministerial Declaration on Universal Access to Immunisation.
President Peter Mutharika and other heads of State from across the continent endorsed the new deal in January during the African Union (AU) General Assembly in Addis Ababa, Ethiopia.
The Addis Ababa Declaration makes universal access to immunisation a cornerstone of health and development efforts.
It was widely hailed as a historic and timely pledge to give every child a healthy shot at life.
In their talks, the leaders saw unrestricted immunisation helping countries reap the benefits of safeguarding every child from preventable infections using vaccines.
As they jetted off filled with optimism and resolve, Moeti rightly warned about the tough task ahead to build on “commitment at the highest levels” to make vaccine-preventable diseases history.
“Putting pen to paper was only the beginning. Now, we must build on the momentum of this historic commitment to create a healthier future for all children in Africa,” she warned.
Africa has improved immunisation coverage in the past 15 years, but progress has slowed.
This is all the more reason governments must back their promise with financial, political and technical resources needed to achieve universal access to immunisation.
Ensuring every child is vaccinated is one of the strategies to transform the country’s rapidly bulging youthful population from a burden on the economy and healthcare system to a healthy working class and wealth creators.
The continent’s immunisation coverage has recently stagnated at 74 percent.
New evidence backed by WHO shows that at the current rate of progress, Africa will miss the Regional Strategic Plan for Immunisation (RSPI) target of reaching the GVAP target by 2020.
A smart start
The words of Ethiopia’s Minister of Health, Professor Yifru Berhan Mitke, ring true.
“Immunisation is one of the smartest investments a country can make in its future,” he told African leaders: “We must do more to protect all our children from preventable diseases not only because it is the right thing to do, but also because it makes economic sense. When our children are healthy, our families, communities and countries thrive.” n





