Falling donor funding: A cost for Africa
Hospice is not just a place to die but funding cuts—and that perception—could be killing our chances of a kinder death as refuges close
The morning sun cuts through half-open blinds and filters into a deserted ward at HospiceWits, the Soweto branch. The rays illuminate a room with five single beds. Bright orange curtains-once drawn to give patients and their families privacy-are roughly knotted or draped over the rails around each bed.
Funding troubles has forced HospiceWits in Soweto to close its in-patient unit. Hlengiwe Dikeledi’s footsteps echo as she leaves the empty 16-bed unit, which closed its doors in July 2017. She is the palliative care manager at the Soweto hospice
“We had to retrench more than 20 people,” she says, “Nurses, cleaners, cooks. Everyone had to go.”
Her office is a small room in what was once an eight-bed paediatric unit-a pastel-coloured paradise. Funding troubles forced the children’s unit to close a year before the adult ward suffered the same fate.
The Hospice Palliative Care Association (HPCA) and its member organisations provide more than 100 000 patients each year with palliative care, helping them to manage the pain associated with life-threatening illnesses such as cancer.
But palliative care is about so much more than what hurts physically. It also supports patients and families psychologically, and even spiritually, to cope with illness and die in a humane way.
Hospice workers mainly provide care in patients’ homes. But in-patient units such as this one south of Johannesburg are important for people who need extra help.
For others, brief stays in hospices can give family members a respite from the 24-hour care many patients need, says chief executive of the HPCA in South Africa, Liz Gwyther.
But the Soweto hospice and over 50 other facilities nationwide were dealt a crippling blow when one of its biggest international donors, the United States President’s Emergency Plan for Aids Relief (Pepfar) reduced its funding by 40 percent in 2014.
Non-profit hospice services took off in South Africa in the 1980s, catering largely for people with cancer and HIV in the era before treatment. As of March 2018, just over 4.2 million people in South Africa were on antiretrovirals (ARVs), according to a department of health presentation to Parliament.
But as more people start HIV treatment and live longer, the US government’s funding focus has gradually shifted from in-patient hospice care towards improving HIV treatment. Aids-related deaths have dropped by almost 60 percent since the government began to roll out free ARVs in earnest in 2007, 2018 SA statistics show.
By contrast, the national cancer registry shows a 30 percent increase in cancer cases between 2010 and 2014. More than 60 percent of patients seen at the HospiceWits were there because of a cancer diagnosis. But after Pepfar support decreased, the township’s only hospice could not raise the R5million (about K2.4 billion) in annual funding to continue to treat patients at the centre, HospiceWits chief executive Jacqui Kaye says.
She adds: “To care for our patients, HospiceWits has to source R32million [about K1.9 billion] in funding each year.”
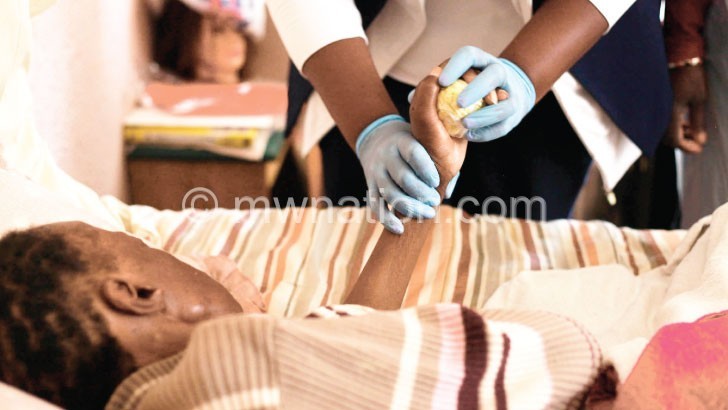
Community caregiver Xolile Dlamini puts a soft plastic ball in 66-year-old Busisiwe Ndimande’s hand to practice her grip as she begins gently rotating her frail wrist as part of regular physiotherapy.
At the start of 2018, Ndimande was diagnosed with late-stage, Alzheimer’s disease, the last phase of a progressive brain condition that causes loss of memory and mental function, according to US non-profit Mayo Clinic.
A 2016 study published in the European Journal of Cancer Care showed family caregivers-even those who had support from people such as Dlamini-reported having a lower quality of life than the general population.
But people who care for sick loved ones and get counselling and support from hospice workers are less likely to become depressed, a 2015 study published in the Journal of Clinical Oncology found.
Under South Africa’s new palliative care policy, home-based care teams will be trained to look after terminally ill-patients at home.
Soweto is not the only community to lose in-patient hospice care as funding dries up. Eight other in-patient units have been closed and several others are on the brink.
Gwyther warns: “We anticipate significant money problems over the next few years.”
Shops selling donated goods bring in just over R12 million per year for HospiceWits. But the rest must be sourced through government, trusts and donations.
“And then there’s the stigma,” Dikeledi argues.
A new national palliative care policy approved last year would help take care out of stigmatised facilities and into communities with local teams treating bed-bound patients in their homes. Palliative care training will also be compulsory at the country’s eight medical schools.
Until then, hospices will be left to brave the competitive world of donor funding and more families will rely on the country’s struggling palliative care facilities.





