Fistula treatment: A healing too far
Women left behind because of aftermaths of fistula cry for greater investment to bring treatment closer to those who need it.
On January 22 this year, Christina Munyoga gave birth to a second baby “mainly to show that she is a woman” like any other.
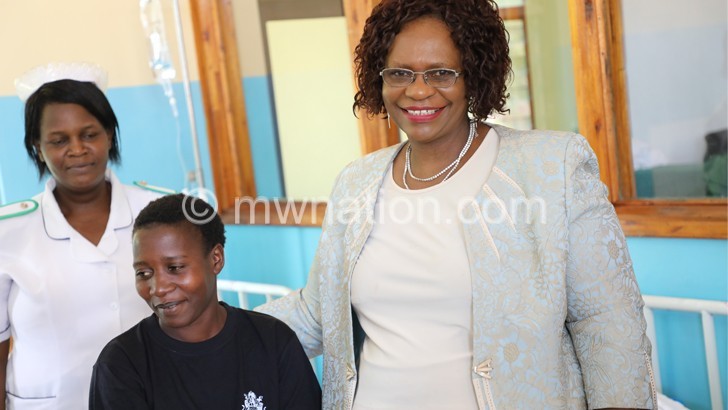
“Seven years ago, my first-born was born through an operation following obstructed labour. After a week, I started leaking urine and faeces. I started wearing nappies like my baby. Following the operation and the hole the baby left in my pelvis, some people mock and shun me. Others call me a lesser woman who couldn’t give birth normally. They say I stink,” she says, with a tear trickling down her cheek.
The 33-year-old, from Liwonde Village in Traditional Authority Mabuka, Mulanje, has survived obstetric fistula—a devastating childbirth injury which left a puncture between her birth canal and rectum.
During a meeting at Mulanje District Hospital, she was among 30 women admitted to await fistula treatment in a camp organised by United Nations Population Fund (UNFPA) last month.
For these women, the road to recovery has been long and winding as fistula treatment in the country hugely relies on the donor-funded campaigns UNFPA rolled out in 2007.
In 2016, Alice Sabuni, 85, put a shocking face to the long waiting list for treatment—having been healed at the first camp in Mulanje after living with fistula for 66 years. The grandmother-of-25 sustained the injury giving birth to her first child in 1949, when she was 17.
The delays continue despite calls for quality healthcare for all, exposing her to untold misery and dehumanising discrimination which deepens poverty.
Munyoga tearfully shares her struggle with atrocities women keep suffering amid slow progress to end fistula.
She narrates: “Most said I stunk. I couldn’t attend group meetings, including village bank meetings where my friends were putting together their savings and sharing soft loans to do small businesses.
“The challenge to do business was torturous. I couldn’t take part in public life. I couldn’t draw water at a public borehole. Even relatives shunned me. Only my husband and child stuck by me for the seven years I was unclean.”
She calls them “seven wasted years”, recounting how fragile fistula treatment and care in the country left her travelling from one health facility to another in vain.
“My husband and I went to Chiradzulu District Hospital, but we were referred to Queen Elizabeth Central Hospital [QECH]. When we got there, doctors said: ‘Come again another day.’ They kept giving us new dates until we couldn’t afford transport to Blantyre. These travels left us without money and time to work in our crop fields,” she recalls.
Just last month, the Munyogas visited Namphungo Health Centre, where medical staff referred her to the treatment camp at Mulanje District Hospital.
“When I heard that a foreign doctor was coming to treat people like me, I thought it was a lie. Then, I heard a similar message on radio. My heart was filled with joy. I couldn’t believe that one day I will be clean—that time will come when I will never be shunned, but interact with anyone and eat from the same dish with those who despised him,” she releases her pent-up excitement.
Her measured words and pensive pauses say it all—she cannot wait for “best thing in my life”.
The weight of this bottled-up joy lies in the number of women grappling with fistula that remain unreached.
The condition “is silently robbing millions of women and girls of their health, hope and dignity,” said UNFPA executive director Dr. Natalia Kanem in her statement ahead of the International Day to End Fistula on Wednesday.
The theme of the observance was ‘Leaving no one behind: Let us commit to ending fistula now!’
However, the UN agency estimates that almost one percent of women in the country are living with the devastating effects of the condition which affects almost two million women globally.
To them, their degrading but treatable condition is a sign of inequality and how the health system is failing to protect the well-being and human rights of the poorest and most vulnerable women and girls.
Ministry of Health and Population Services spokesperson Joshua Malango commends UNFPA and Freedom from Fistula Foundation for flying in foreign surgeons and supporting government’s efforts to liberate affected women one surgery at a time.
Interestingly, the ministry knows that training local health worker to conduct repair surgeries would be three times cheaper.
“The fistula treatment camps are expensive,” he says. “Flying in foreign doctors is costly. Besides, for a patient to be fully managed, we spend approximately $1 200 compared to about $400 if we provided routine care.”
But Malango sounds optimistic as the camps offer Malawian clinical staff hands-on training.
“During the camps, local doctors and clinical officers are also trained in the surgical procedures to handle uncomplicated cases. Currently, we have almost 10 providers trained in that way. Complicated cases are referred to Bwaila Fistula Centre in Lilongwe,” he explains.
The 10 handle minor cases at Mangochi, Mulanje, Chikhwawa, Zomba and Nkhata Bay district hospitals where they handle uncomplicated cases. Guidelines require district health management teams to promptly refer those diagnosed with complicated obstetric fistula to Bwaila.
“As a country we are trying as much as possible not to rely on obstetric fistula camps. Camps are being conducted only when we have complicated cases, especially where they have no skilled providers, infrastructure and equipment to provide the service.
“For one to competently operate on a complicated case, he or she needs to specialise in the field. Currently, we don’t have such personnel,” says Malango.
The stand is echoed by Mulanje district health officer Dr Khuliyena Kabwera.
“We need a special theatre and skilled health workers for fistula treatment. There is always skills transfer and the camps are helping build the capacity of our staff. So far, we have one trained clinician who conducts fistula repairs, a step towards lessening the suffering of women in need of treatment. However, it depends on the degree of the cases. We refer complicated cases to QECH in Blantyre and Bwaila in Lilongwe for specialised treatment,” he says.
The trained clinician in Mulanje works in an overwhelmed general theatre.
“Apart from training more skilled hands, we need assistance to establish a special theatre for fistula. There is scramble for the general theatre. When there is an emergency case, we stop assisting fistula clients,” Kabwera narrates.
The constraints and SOS mirror a long way to end over-reliance on external assistance.
And there seems to be no end in sight.
“We will still be relying on foreign experts to operate on complicated cases until we have our own doctors specialised in the field,” declares Malango.
Nonetheless, he bills the situation “better off” because there are a few officers who can treat minor cases and some hospitals with surgical equipment, supplies and trained midwives to manage fistula clients before and after repair surgeries.
But some women with fistula go undetected due to widespread stigma.
In what Minister of Health Atupele Muluzi terms “doing more with less”, district hospitals rely on health surveillance assistants (HSAs) to identify and refer them to treatment sites.
UNFPA Malawi representative Ratidzai Ndhlovu commends the treatment camps for “doing a lot to restore the dignity of women and girls” who feel humiliated and excluded.
When asked about the state of care, she explains: “The visiting surgeons work hard with the locals for skills transfer. They are doing a lot to restore smiles on the faces of women, even those abandoned by their husbands. The foreign experts do the procedure and leave, but the locals remain behind to do minor procedures.”
“We are not there in terms of treatment, but we will get there. We need to do more to support our surgeons and to take treatment closer to women and girls who spend many years looking for it. We can do something about it.”
After the long-awaited procedure, Munyoga sympathises with unreached women who are stuck in poverty due to fistula at a time Sustainable Development Goals require countries to leave no one behind even in terms of access to healthcare services.
“I will be glad to go home healed and smiling, but some women and girls are still suffering in isolation because they do not know where to go or their nearest health facility only offers tablets and injections that cannot cure them,” she says, with a fading smile her husband Charles admittedly got accustomed to in the past seven years.
Seven years constitute half the age of Funny Nyambalo, who quit school because she could not bear the insults, seclusion and low self-esteem that living with fistula entails.
“Some laughed at me. Others fled from me. Only my parents showed me love and supported me to get treatment. When I go back home, I will go back to school because I want to be a doctor to assist those who need treatment, especially women and girls with fistula,” says the 14-year-old, from Makuwa Village in T/A Mabuka.
But there is a deeper cry in her measured voice of agony and renewed dream: Malawi needs to train more skilled hands to liberate women and girls long held back by fistula.