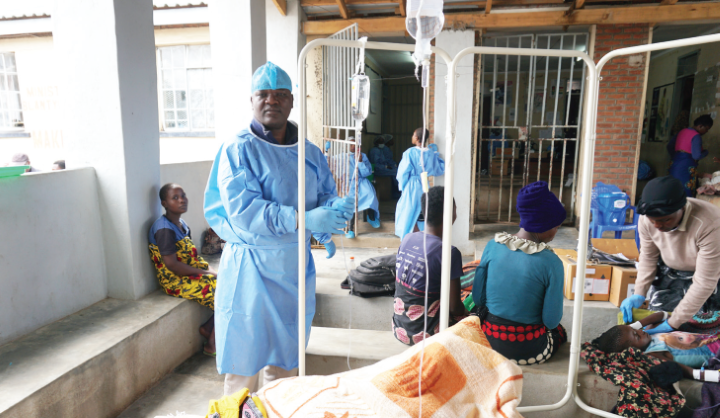
Judged, shunned, at risk
Sex workers want an end to discriminatory tendencies constraining access of healthcare services. JOHN CHIRWA writes.
She does not want to be named.

“Please, don’t mention my real name because my parents and clients will not be pleased,” pleads a youthful sex worker disguised as Mary.
It is a condom burst in 2014 that she loathes the most, she says.
“Health workers at Mzuzu Central Hospital were unwilling to attend to me when I contracted a sexually transmitted infection following the burst. I was told to bring my partner, but I told them it was almost impossible to trace the client,” she explains, accusing clinicians of shunning her because she is a sex worker.
The symptoms of her infection reportedly appeared two weeks after the condom breakage, probably the reason she is HIV positive today.
She hooked five short-time clients on the dreadful night, she says.
Being known as a sex worker often attracts derogatory names from health workers, pushing them not to seek treatment on time.
“Hospital staff often accuse us of spreading diseases, especially HIV and Aids” she says.
Untold stigma forced her to seek treatment at private clinics.
She says she did not choose to become a sex worker.
“Circumstances forced me into this,” says the divorcee.
The mother of a seven-year-old girl ventured into the trade when her marriage collapsed three years ago in Lilongwe.
She returned to her parents’ home at Chibavi in Mzuzu. But her parents separated in no time, piling pressure on her to support her child singlehandedly
She began hanging out “once in a while”.
Today, Mary says sex work is the only thing she does to support her life and child in the city with the third-largest population of sex workers countrywide.
She is just one of over 20 000 sex workers nationwide who are highly at risk of contracting HIV.
Out of 100 sex workers, almost 62 are reported to be infected.
This is about seven times higher than the national prevalence estimated at 8.8 percent, according to the Malawi Demographic Health Survey (MDHS).
Youth and Society (YAS) gender and child rights officer Linda Sichali urges public health providers to leave no-one behind as the world pushes hard to ensure that 90 in every 100 people know their status, 90 in 100 diagnosed with the virus recieve antiretroviral treatment and 90 percent of those on ART treatment achieve lowered viral load.
“There is need to embrace diversity and respect of the rights of all-even the under-represented and most-at-risk groups-as the country races towards the 90:90:90 global target,” says Sichali.
Sex workers are among most-at-risk groups, which include drivers, prisoners and migrants as well as lesbian, gay, bisexual, transgender and intersex persons.
“If we leave sex workers behind, then Malawi will not reach its target because they are a minority with a majority client base. Some of their clients are husbands, the clergy and traditional leaders who may infect their stable sexual partners as well,” she explains.
YAS and Family Planning Association of Malawi (Fpam) are working together to close the gaps through Differentiated Care Project funded by International Aids Society.
The civil society organisations conduct focus group discussions and trainings which offer sex workers a safe space to access HIV services, including condoms, testing, treatment, care and STI screening.
“To protect the majority, we want this minority group to be empowered on protection, treatment and adherence to medication,” she says.
However, National Aids Commission (NAC) spokesperson Felix Thawani recently called for intensified efforts to reach out to populations left behind in the HIV and Aids response for the country to achieve zero discrimination, zero new infections and zero Aids-related deaths.