Malaria vaccine on trial
It’s World Malaria Day. Our Staff Writer JAMES CHAVULA unpacks malaria vaccines on trial in 11 districts.
It is a warm evening and you are having a mealtime chat with your family. All looks pleasant as you unwind from a busy day, probably listening to soothing music or news. Suddenly, there is a piercing sound in the air and then comes an excruciating sting in some exposed skin.
Ouch! You slap the stinging spot with unrehearsed promptness, crushing the buzzing bloodsucker causing pinpoint pain to your exhausted flesh in need of relaxation, not the horrors of mosquito bites.
Little bloodsucker. You rub off the mosquito and bloodstains, worried that it might have infected you with malaria.
Such is an everyday risk faced by many people in Malawi where health facilities treated about five million malaria patients in 2017.
The majority of the population estimated at 17.6 million grows up hearing that the war on malaria will be won by sleeping in mosquito nets treated by insecticides, but they are often exposed to mosquito bites before slipping into the nets distributed free of charge to pregnant children and women. At worst, mosquitoes, which multiply and lurk in damp spaces, attack them without a buzz.
New vaccine
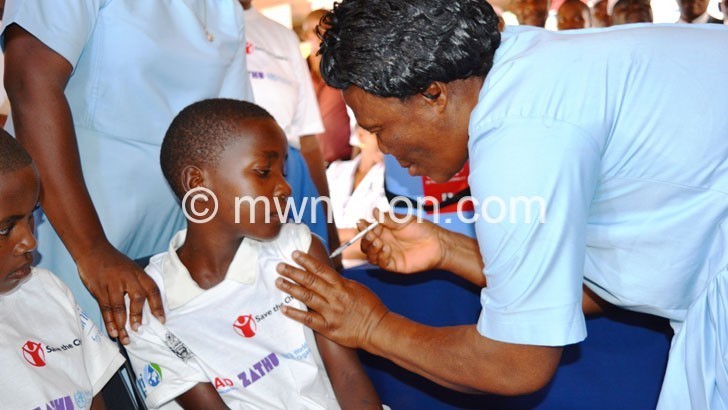
However, the good news is that nearly 120 000 children the size of Dorica Julius’ four-month-old twins are poised to receive a vaccine which nearly halves the risk of getting malaria. The vaccine offers relief to people like her.
“When a child is taken ill by malaria, I leave everything I planned to do and travel over two hours to receive medical care at Gaga Health Centre, where we queue for an hour or two. At times, the baby is sick for a whole week, shivering and vomiting,” says Julius, who lives in Chapananga in Chikwawa.
On Tuesday, the Ministry of Health in partnership with the World Health Organisation (WHO) and Path Malaria Initiative rolled out pilot tests for the world’s most effective malaria vaccine in the worst hit districts like Julius’. Apart from Chikwawa, they include Karonga, Nkhata Bay, Ntchisi, Mchinji, Lilongwe Rural, Balaka, Machinga, Mangochi, Phalombe and Nsanje.
There will be similar trials in Kenya and Ghana where malaria transmission remains high despite a history of using insecticide-treated nets.
The vaccine stimulates the body to fight the disease that causes about 60 percent of deaths in children aged five and below in Malawi.
According to WHO, Mosquirix, created by drug scientists at GSK in Britain is a result of three-decade-old experiments worth $1 billion.
In 2015, the United Nations (UN) health agency approved the vaccine which offers lower immunity than those of other diseases. However, at 40 percent, Mosquirix is billed the world’s most effective malaria vaccine.
Scientists believe that partial protection will avert hundreds of deaths caused by the disease haunting a third of patients that queue for treatment in the county’s health facilities.
The immunisation campaign will supplement mosquito nets in wiping out malaria.
“Besides the existing malaria interventions, new complementary tools and strategies are needed to accelerate the fight against malaria,” says Ben Chisamire, the chief director at the Ministry of Health.
Malaria can kill a child in less than 24 hours, a scientist warns.
“Even if the child survives, malaria can impact every organ, causing brain injury or even kidney issues. Prevention is better than treatment,” researcher Tisungane Mvalo, a paediatrician at University of North Carolina at Chapel Hill Project-Malawi in Lilongwe, told AFP.
Malaria cases in Africa are on the rise. WHO reports that the number of malaria cases jumped by over two million between 2016 and 2017, though the death rate has fallen nearly two-thirds since 2000.
Last year, the African Union’s Centre for Disease Control and Prevention (Africa CDC) worked closely with the neighbouring Mozambique to mind and analyse long-term data which revealed “a silent outbreak”.
Despite efforts to combat malaria, the situation in Mozambique revealed a larger public health concern concealed by gaps in data management,” says Dr Mazganga Mazaba, a research and communication officer at Africa CDC regional collaborating centre in Lusaka, Zambia.
According to the Ministry of Health, new methods are needed to end malaria transmission which often peaks during the rainy season, from November to April. The disease burden is high in lowlands along Lake Malawi and Shire River.





