Malawi on course to end Aids, but…
For the man we have disguised as Amon Maliseni to conceal his family’s identity, the virus is not the end of life or marriage.
He has been supporting his wife who was diagnosed with HIV the day their third child was born.
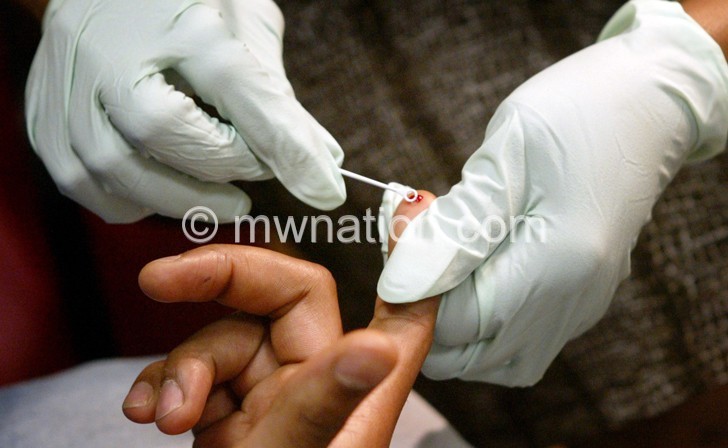
“I vowed to treasure her for better and for worse. What we are going through is a test of our love and the time to show the strength of our bond,” says Maliseni.
He contrasts sharply with her first husband, who walked away—abandoning the woman and their four children as opportunistic diseases kicked in. Maliseni has stuck by her even though he was diagnosed HIV-free several times.
The discordant couple—an intriguing rare condition where one partner is HIV positive and the other is not—says they will only be parted by death.
“When she told me about her status, I didn’t take it for granted that I may also be positive. So I also went for HIV testing as advised by a counsellor who comes to encourage couples affected by HIV to a skilled clinician in case of any danger sign. I didn’t know how to react when they couldn’t detect the virus in my blood. I didn’t know how to react,” explains Maliseni.
He says knowing their status has helped them support each other to live longer. Together, they had three children, but one died.
The family of subsistent farmers, who cultivates a field smaller than a football ground, hugely survives on piecework in their well-off neighbours’ gardens. Last year, they were hit hard by food crisis caused by drought in the Shire Valley, which forced her to stop taking antiretroviral drugs (ARV).
During our visit to Nsanje District Hospital where his wife was admitted, the man was away doing piecework in homes and shops in the vicinity to provide for the tuberculosis patient and her guardians.
Treatment too far
This illustrates the financial hardship patients and guardians from remote areas bear to access treatment for Aids-related illnesses.
Nowadays, government is promoting universal health coverage to ensure everyone gets quality assistance when they need it, where they live and without worsening poverty. But in rural settings where Maliseni and 84 percent of the population live, health facilities are few, far between, understaffed and lacking essential equipment and supplies to detect and treat advanced HIV conditions.
The income generating activities Maliseni does to support his wife and her guardians during the hospital stay demonstrate her fitness.
“I do any work that comes my way, including clearing crop fields in preparation for the next growing season and tidying up lawns and backyard gardens,” he explains.
Maliseni thanks his wife for helping him go for testing and he uses condoms to protect himself.
He reckons many adults living with HIV keep their status to themselves for fear of being abandoned by their spouses.
He warns against stigma and discrimination, saying it prevents infected people from getting tested and commencing treatment.
National response
The country has adopted a new post-testing policy that requires those found HIV positive to start taking ARVs straightaway regardless of their status.
This builds on the successes of efforts to ensure every pregnant woman gets tested and starts taking the drugs instantly if found positive.
This has proved a major leap in prevention of mother-to-child transmission. The Ministry of Health credits the strategy with over 90 percent reduction in newborns’ infection rates.
This represents a big boost since 2005 when frequent deaths and debilitating illnesses compelled government to roll out free access to ARVs.
National Aids Commission (NAC) spokesperson Karen Msiska says the annual count of Aids-related deaths has dropped from 64 200 to 13 000 for the past 15 years.
The breakthroughs in testing and treatment have motivated the Ministry of Health to extend the test-and-treat policy beyond pregnant women and those with high viral load or CD4 count.
Globally, Malawi is billed a star performer in the United Nations (UN) Start Free Stay Free and HIV Free initiative to enhance life-saving actions in 23 countries with high numbers of children, adolescents and young women living with HIV.
According to a new report by the UN Joint Aids Programme (UNAids), fewer children newly infected with HIV and improved health for mothers living with HIV stand out as achievements of the global Aids response in recent years.
The new evidence reads: “This has been done by dramatically increasing the proportion of pregnant women living with HIV receiving antiretroviral medicines from 43 percent in 2010 to 85 percent in 2018. This was a significant achievement, but the 2018 target of 95 percent coverage was missed in all but five focus countries—Botswana, Malawi, Mozambique, Namibia and Zambia.
Save for India and Indonesia, all the countries in focus are located in Sub-Saharan Africa.
On course to end Aids
In the worst hit region, Malawi’s strides points towards a winning battle to end Aids—an acute drop in body defences to deadly diseases, including tuberculosis and meningitis which kill about half of people with HIV.
A new study Amfar Institute for HIV Cure Research and Friends of the Global Fight against Aids, TB and Malaria unveiled this week at the International Aids Society (IAS) science conference in Mexico, ranks Malawi in the top six countries on course to end Aids by 2030. Other countries on course to achieve the UNAids’ 90-90-90 targets are Uganda, Thailand, United Kingdom, Australia and San Francisco, US.
The global agenda to end Aids by 2013 requires countries to ensure 90 percent of people infected with the virus know their status, 90 percent of those with the virus start taking antiretroviral medicines and 90 percent of those on treatment take it consistently to reduce the viral load to undetectable levels.
In the wake of the findings, Dr Charles Mwansambo, chief director of health services in the Ministry of Health, told The Nation that by March 2018, the country has tested 91 percent of people suspected to be HIV positive, with 86 percent of those found HIV-positive receiving the life-prolonging drugs and 90 percent of those on treatment achieving suppressed viral load.
“This is an exciting progress we should guard jealously,” he said. “This means that out of almost one million Malawians that are living with HIV, by end of March 2018, an estimated 750 000 people were on treatment, out of whom 86 percent have had their viral load suppressed, thereby reducing the risk of transmitting HIV to their sexual partners or from mother to child.
But Mwansambo warned that progress “will not be sustained if we continue to have new HIV infections estimated at nearly 38 000 a year. This means 104 people in the country acquire the virus every day, with one getting infected every 30 minutes.
“We need to jealously guard our success,” says Mwansambo.
New science also reveals that apart from prolonging the life of a person infected with HIV, taking ARVs consistently until the virus becomes barely visible eliminates chances of transmitting the virus to a sexual partner.
Challenges remain
Despite this progress, HIV remains the leading killer among adults—causing nearly 17 000 deaths in Malawi every year. This means it costs about two lives per hour or three deaths by the time a football referee blows the final whistle.
According to Medecins Sans Frontiers (MSF) country representative Ilse Casteels, the country needs to intensify efforts to end deaths from conditions catalysed by advanced HIV.
“Despite the impressive strides, challenges remain as 21.7 percent of HIV patients still don’t know their status and a significant number of patients has interrupted their treatment and are lost to follow up. Other patients are failing on treatment, but only low proportion of them has been switched to the second line ARV,” she explains.
Maliseni’s wife is a TB patient, which causes a third of deaths related to Aids. This makes the respiratory disease the main killer of people with HIV ahead of meningitis which kills a fifth.
Dr Gilles Van Cutsem, leader of MSF HIV/Aids working group, says more needs to be done to confront the killer infections driving Aids-related death, starting with tuberculosis and meningitis.
“In MSF supported hospitals in the Democratic Republic of Congo, Guinea, Malawi and elsewhere, many deaths occur within 48 hours of admission,” explains Cutsem. “Patients arrive very ill, often with severe opportunistic infections such as tuberculosis, cryptococcal meningitis, or Kaposi’s sarcoma. When they arrive, sometimes it’s too late to save them. They might not have been diagnosed on time, or failed to get access to a life-saving treatment.”
‘We can’t celebrate’
The deaths are primarily driven by delayed diagnosis and treatment interruptions. WHO estimates that more than 30 percent of people who start HIV treatment worldwide have severe loss of immunity which exposes them to deadly opportunistic infections.
Explains Cutstem: “Many patients go first to primary healthcare centres when they feel sick. If primary care clinics are not equipped and trained to detect advanced HIV, patients at risk will remain undetected and untreated; they will deteriorate until they are terminally ill. Then some will be referred to hospitals often missing the basic tools to manage them.
“We cannot celebrate or talk of success while hundreds of thousands continue to die of Aids every year because they do not access basic HIV care.”





