Rising above hopelessness to avert baby deaths
When the World Health Organisation (WHO) ranked Malawi as leading the world in the highest rate of premature births at 18.1 for every 100 births two years ago, it must have set the despair gong off in a country already reeling from a battered maternal health image.
Further revelations in the WHO’s 2012 report titled Born too soon: The Global Action Report on Preterm Birth that these births account for almost half of all newborn deaths worldwide and are now the second leading cause of death in children under five after pneumonia offered little hope to this sub-Saharan nation.
The report attributed serious complications such as infections and respiratory distress as the major causes of deaths in premature babies while countless others suffer some type of lifelong physical, neurological or educational disability, often at great cost to families and society.
Although WHO admits that many preterm births remain unexplained, it said the main causes of preterm births in many low-income countries are infections, malaria, HIV and high adolescent pregnancy rates.
Maternal health complications are many and they account for 460 deaths per 100 000 live births according to fig.org. UNFPA places the neonatal mortality at 30 deaths per 1 000 live births in the country. Respiratory distress claims the lives of about one million African babies each year.
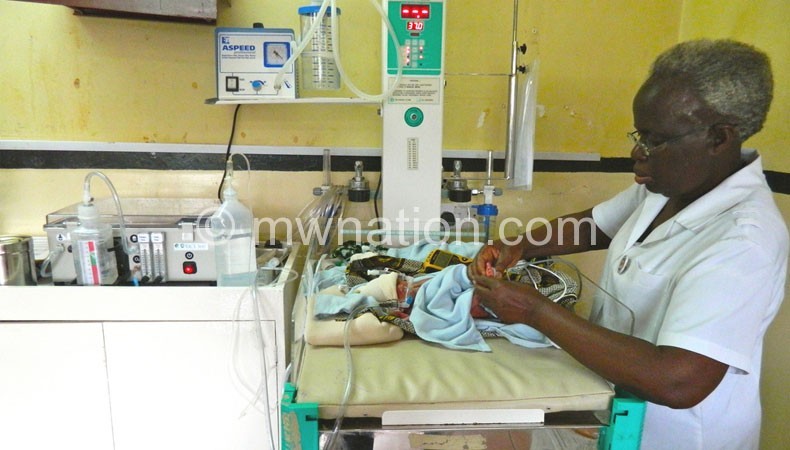
Oblivious to the WHO report, Friends of Sick Children (FSC) at the paediatric section of one of the major referral hospitals in the county, Queen Elizabeth Central Hospital (QECH), concerned about the high rate of respiratory distress in premature and neo-natal babies devised an innovation to fight infant mortality rate.
The innovation, a life-saving kit called ‘bubble’ Continuous Positive Airway Pressure (‘bCPAP’) aids breathing in babies that are in respiratory distress, won the best global recognition by GlaxoSmithKline (GSK) and Save the Children Healthcare Innovation Award for its high quality, affordable and replicable package of treatment services.
The low-cost device that started out on a mere trial basis could now prevent 178 000 early neonatal deaths per year in Africa, placing Malawi on a pioneering platform towards winning the battle against premature deaths.
The device again offers hope to achieving the UN Millennium Development Goal (MGD) 4, a two thirds reduction in young child deaths and goal five; improved maternal health by 2015 for many African countries.
FSC, a partnership between the Paediatric Department at Queens, University of America’s Rice 360Ú Institute for Global Health Technology and University of Malawi’s College of Medicine are the brains behind bCPAP.
This device aids babies by keeping their lungs inflated so they can breathe more easily. Newly born babies are usually placed on the machine for two to five days and one to four days for older babies.
bCPAP engineer at Queens Jocelyn Brown said one or two out of 10 babies born premature require respiratory support. She said the device has significantly reduced infant mortality.
Brown said upon successful trials in Malawi, bCPAP is expected to be rolled out in teaching hospitals of Tanzania, Zambia and South Africa.
“Queens was the first hospital to use the device in 2012 and is now operational in four central hospitals of Blantyre, Lilongwe, Zomba and Mzuzu,” said Brown.
She also said that bCPAP is benefiting babies in five district hospitals across the country with 27 district hospitals lined up once fully fledged.
Brown said benefiting hospitals were identified by the Ministry of Health to be carried out in a three-year period in three phases. The hospitals include QECH, Kamuzu, Zomba and Mzuzu central hospitals; and those in Mwanza, Machinga, Bwaila Maternity Wing, Kasungu and Rumphi.
The genesis of bCPAP, according to Brown, is a visit to Malawi and other African countries by two bio-engineers from Rice Rebecca Richards-Kortum and Maria Oden.
She said the two women went about asking doctors the kind of technology they would want for their hospitals and QECH chose a device to aid respiration in newly born babies.
Brown said it was then that she and other students at Rice got down to work and developed the bCPAP, a mechanical device which cost less than $500 (about K215 000), a 15-fold reduction from the average cost of devices currently used in developed countries where they cost at least $6 000 (K2 580 000) each.
“Part of the $400 000 [K172 million] prize money from the award will be used to purchase bCPAP supplies, trainings and transportation to Tanzania, Zambia and South Africa,” said Brown.
At the announcement of the winner in November last year, Save the Children and GSK said in a press statement that innovations such as the bCPAP device demonstrate how countries are finding their own solutions to their biggest problems.
The bCPAP device as one of the five projects from a long list of nearly 100 applications from 29 countries across the developing world selected by the judging panel, according to the statement.
The GSK and Save the Children $1 million (about K430 m) Healthcare Innovation Award fund was set up to identify and reward innovations in health care that have proven to be successful in reducing child deaths in developing countries.
According to more than 100 experts from 40 UN agencies, universities and organisations who contributed to the WHO report, the top 10 countries with the highest rates of preterm births for every 100 births are Malawi with18.1 per 100 followed by Comoros and Congo at 16.7, Zimbabwe at 16.6, Equatorial Guinea at 16.5, Mozambique at 16.4, Gabon at 16.3, Pakistan at 15.8, Indonesia at 15.5, and Mauritania at 15.4.
Experts at the UN, medical institutions and field organisations say that inexpensive, proven forms of care for premature babies could save at least three quarters of these babies in the developing world.
It said a number of countries such as Ecuador, Botswana, Turkey, Oman and Sri Lanka have halved their neonatal deaths from preterm birth through improving care of serious complications like infections and respiratory distress.




