Slow prep for zero HIV in women
HIV in Malawi has a woman’s face because she remains exposed to the virus, with girls aged 15-25 demonstrating almost four times the number of HIV cases among their male age mates, JAMES CHAVULA writes:
A woman renamed Maria Mwale, in her 40s, feels women are lagging behind despite their iconic role in efforts to combat the HIV and Aids pandemic.
“A woman has been at the centre of nearly every trial and breakthrough, but we are not really doing enough to protect her,” she says.
The mother-of-one, from Bvumbwe in Thyolo, was diagnosed with HIV in 1998.
That was seven years before the rollout of free antiretroviral drugs (ARV) for all in 2005.
“I was young and still in school. We didn’t know the drugs existed. We started hearing news of ARVs in 2000, but we didn’t know where to get them. We couldn’t afford a pill,” she recalls.
Counting the gains
The National Aids Commission (NAC) reports that liberalised access to the drugs has reduced the count of Aids-related deaths in the country from 64 000 to just about 13 000 a year for the 15 years she has been on treatment.
She feels healthier than expected, saying: “The amount of HIV in her body cannot be detected, if you look at me, you wouldn’t know I have the virus.”
The advancement in HIV treatment includes the screening of every pregnant woman. Those living with the virus are instantly put on lifelong treatment enjoy a healthy life and give birth to HIV-free children.
Looking back, Maria states: “If it was available when I got pregnant as a Form One learner, I wouldn’t have suffered stigma because I knew my status when I was wasting and the boy was born HIV-positive. The man I married after my husband’s death fled from me because I was sickly.”
In 2016, the Ministry of Health expanded the treat-all approach to the entire population regardless of sex and age.
Dr Dan Namarika, Principal Secretary for Ministry of Health, says the test-and-treat plan, in which those diagnosed with the virus are immediately put on treatment, has helped avert the horrors of the pandemic.
To him, increasing the population of people getting tested and treated helps them live longer without transmitting the virus.
“The change [in the number of death per year] is so dramatic, every family feels it,” he says.
However, is concerned that new infections are increasing faster than expected because people no longer experience Aids as they did when coffin workshops chocked every street.
New challenge
As a member of the Global Coalition on HIV Prevention, Malawi this year has missed to reduce new infections by 75 percent from 59 000 to 11 000 since 2010.
Last year, the Ministry of Health reported that 38 000 people had contracted the virus in 2018—up from 36 000 the previous year.
This has turned up calls for increased focus on HIV prevention, especially among adolescent girls and young women who are twice as likely as their male peers to be living with the virus.
“There is need to expand the prevention tool box, particularly for women who only rely on a condom currently,” says Ulanda Mtamba, an ex-fellow at Avac. “Globally, women have participated in different research, but the processes to get the final results are too slow for some products which might benefit women.”
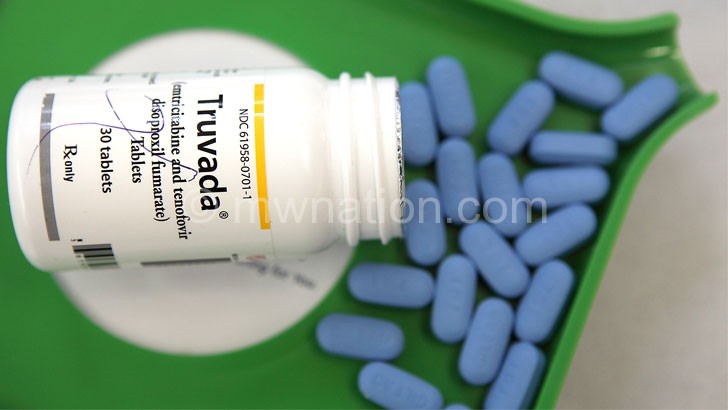
She asks government to accelerate the use of new technologies that are already out of the pipeline—including pre-exposure prophylaxis (or PrEP), ARVs taken by HIV negative people to prevent HIV infection is not readily available across the country.
Trials by World Health Organisation (WHO) in Africa, Asia, Europe, North America and South America showed that it reduces the risk of getting HIV from sex by 90 percent when taken once a day for at least 20 days.
The Ministry of Health approved PrEP for HIV prevention in December 2018, but the pill is not readily available in public facilities.
Activists feel the expansion of access to PrEP is too sluggish—much slower than the adoption of medical circumcision which reduces men’s risk of acquiring HIV by 60 percent, according to the World Health Organisation (WHO).
Mtamba asks: “Why is it that governments that were quick to adopt tools that protect men grow cold feet when it comes to more effective technologies likely to protect women?
“Despite the high new infection rates among women, there are preventive measures which are already out, such as PrEP, but policymakers are still dragging their feet to accept tools that would give women the power and privacy to control their sexual health.”
The pro-women technologies still on trial include a virginal ring, which slowly releases preventive medicine for 30 days when it is supposed to be replaced.
Since 2013, the University of North Carolina has been running clinical trial on the impact of the microbicide ring, which is supposed to be replaced every month. Results released in October shows it reduces the danger of contracting the virus by up to 73 percent, Dr Tchangani Tembo says.
According to the coordinator of the Aspire Study, the ring is awaiting government’s approval.
“Women need to embrace the technology once it hits the market because it can reduce HIV transmission,” he says, explaining: “Once inserted in the vagina, the ring slowly releases the drug to prevent the acquisition of HIV. Form the trials, it has proved to be effective.”
Scaling up
When asked about the new innovations, Namarika said: “We haven’t done much on the ring, but we have embraced PrEP, though not fully. The Ministry of Health is working with FHI 360 and other partners to pilot PrEP among key populations, especially sex workers and adolescent girls and young women.”
He said lessons from the trials underway in parts of Blantyre, Lilongwe, Mulanje, Phalombe and Machinga will clarify what the country can do or not when it expands the programme to all districts this year.
“So far, we have learnt that we can protect many people by protecting one person at risk, including female sex worker who say they sleep with three or four men a night,” he says.
At Kachere Township in Blantyre, we met a sex worker, who is distributing PrEP, condoms and lubricants in her room in a discreet peer-to-peer project run by Pakachere Institute for Health and Development.
She explains: “My room is a mini-clinic. Colleagues who love life come here day and night to pick what they need to protect themselves. Those who don’t, my friends and I go to them to remind them that we only live once.
“Ours is a risky trade because we meet men who offer a lot of money for unprotected sex if you insist on condoms. You cannot tell whether they are living with a virus and they don’t care whether you are infected. Fortunately, no one will know if you take PrEP.”
She likened PrEP to injectable contraception, saying both sex workers and people in risky stable relationship can take it with maximum privacy and confidentiality.
This personifies how the new drug could help women take control of their sexual life at a time stable relationships, including marriage, have become minefields of new infections.
Scientists warn that the pill does not replace the current HIV preventive measures but supplements condoms, circumcision, antiretroviral drugs and prevention of mother-to-child transmission.
Besides, they say, it does only protect one from HIV, but also sexually transmitted infections.
However, UNAids PrEP expert Rosalind Coleman says: “The link between PrEP and increase in other STIs beyond is a hot topic, but the discussion should not become a reason to reduce PrEP access. Instead, it should identify and encourage improved comprehensive sexual health services for prevention, identification and treatment of all STIs.
“The most recent systematic review confirmed that the STI rate already high in people asking for PrEP, which is to be expected, and confirms that the people asking for PrEP are having condomless sex.”
To Mtamba, the slow uptake of innovations likely to safeguard a woman from HIV somehow reduces her opportunity to a test kit.
It further slows the race for—prevention—a silent 90 in the 90-90-90 goals to end Aids by 2030.
The global targets backed by UNAids required countries to ensure 90 percent of people living with HIV know their status, 90 percent of them start taking treatment consistently and 90 of those on treatment achieve a state where the amount of viruses in their bloodstream is neither detectable nor transmittable.
Recent assessments show the country has scored 92-84-91 in the race to end HIV, meaning it has come six percentage points short of the second 90—increasing access which has become handy in HIV prevention.
However, Maziko Matemba, board chairperson of Malawi Network of Aids Service Organisations (Manaso), urges caution.
He said: “We really need new innovations for at-risk populations, including women. We are not doing well in terms of prevention as we rely on donors who focus more on treatment side.
“However, we need to critically look at the new technologies so that we don’t adopt methods that people won’t accept or those we cannot sustain without donors’ goodwill.”
But women’s vulnerability to new infections are compounded by a culture of silence, with those who speak up often perceived as promiscuous.
At worst, nearly four in five women suffer sexual violence often orchestrated by people they trust, including spouses, boyfriends or intimate partners.
“Abused women, especially adolescents and young women have little or no power to bargain for safe sex, increasing the risk of HIV,” says medical officer Bertha Mvula, based in Mulanje where one in five people live with HIV. n





