Space crisis in hospitals
A rise in referral cases to the country’s four central hospitals has clogged the facilities so much that in the wards all space on the beds and floor is taken up.
Consequently, some patients are forced to occupy corridors.
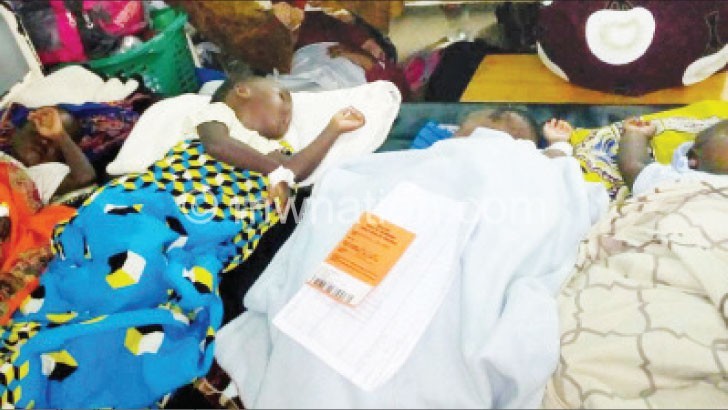
Congestion is most pronounced at Queen Elizabeth Central Hospital (QECH) in Blantyre, the country’s largest referral hospital with 1 200 beds.
Its winding corridors leading to the wards that are perennially congested— where patients share beds and sometimes the floor—are being used as make-shift wards.
This sorry state, exacerbated by underfunding, rise in cancer cases, malaria and diarrhoea outbreaks and lack of health personal at district hospitals, is replicated in the other referral hospitals in the country—Kamuzu Central Hospital (KCH) in Lilongwe as well as Mzuzu and Zomba central hospitals.
According to hospital administrators at QECH and KCH, congestion is aggravated by a weak referral system to central hospitals in the districts that do not have their own public district hospitals.
Amos Nyaka, Society for Medical Doctors (SMD) president said Malawi has a health system that is clogged at the top, leading to poor services, overcrowded facilities, overworked medical staff, and, as a result, medical malpractices such as misdiagnosis.
“Overcrowding versus staff shortages in our hospitals can be very challenging,” said Nyaka who leads a grouping of medical doctors operating in the country. “It is challenging to communicate sensitive information to patients. Some patients might even get discharged while still requiring admission because of the need to admit other even very sick patients. Patients may be at risk of cross transfer infections and at the same time health workers are equally at risk of nosocomial [hospital-acquired] infections.
“Overcrowded health facilities also make Malawian health workers the most over worked civil servants. It is very challenging to work in such environments,” Nyaka said, suggesting that the problem could be eased by constructing new facilities and expanding the existing ones.
Treasury spokesperson Davis Sado said government allocated K4 billion to the referral hospitals which could have been used to increase bed space.
“In the 2017/18 budget, a total of K4 billion was allocated for operations of central hospitals. It is, therefore, the responsibility of the ministry [of Health] to allocate the resources at a cost centre level and to specific budget lines including the line of beds,” Sado said.
Worst affected
At QECH’s 2A Ward, patients—some of them critically ill—are exposed to prying eyes of the public trying to negotiate their way around a maze of mattresses in the corridors. Some patients—with glucose and blood drips leaning against the corridor walls—are a sorry sight requiring special care in a closed room.
The hospital is a flat single storey building, connected with covered walkways, stretching over a kilometre of fenced-in area with 1 200 bed space yet it accommodates over 1 500 patients.
Opened to the public in 1958, QECH registers 1 000 births a month and the paediatric department alone admits 100 000 children a year with various illnesses, including malnutrition, malaria and gastritis.
Douglas Manjilili, a guardian who came with a patient from Mulanje, said in an interview on Tuesday, that some patients feel hopeless because of the congestion.
“The situation is pathetic and hopeless. Patients are not safe in the corridors. There is no privacy. They have to receive medication or change their clothes in the full view of other patients and guardians,” he said.
Manjilili said there have been cases where patients are trampled on as people pass through.
In a telephone interview on Wednesday, the hospital’s administrator Themba Mhango said the situation of patients sleeping in the corridors was compounded by the fact that an additional ward is still under construction.
“The patients that are now being accommodated in those places, such as wards 2A and 4B, should have been moved to the new ward. Unfortunately, the contractor is yet to handover the building to the ministry, for our use.
“But what I can say is that the overcrowding of patients has also been because of the new cancer screening services that we are now offering. This has resulted in overwhelming numbers of cancer-related cases being referred to this facility,” he said.
Malawi Cancer Registry statistics show that QECH records an average of 18 to 22 cases per week—averaging 72 to 84 cases per month.
However, Mhango agrees that the conditions the patients are exposed to in the corridors are not suitable for a functioning healthcare system.
“There is no privacy when doctors are examining patients and also diseases such as cancer require that patients on medication must be accommodated in places that meet international health standards,” he said.
Cross-cutting problem
Congestion is not different at Zomba Central Hospital, KCH in Lilongwe and Mzuzu Central Hospital, where Weekend Nation visits showed that the hospitals’ facilities and resources are stretched to crisis levels.
According to government Annual Economic Report for 2017, in 2015/16, on average all public hospitals registered 843 189 admissions of which 17 699 patients died. While out-patient department (OPD) utilisation stood at 17 065 044 attendances.
The situation at KCH defies the universal definition of primary health care, provision of basic curative health services on the basis of community participation and inter-sectoral collaboration. Congestion is a serious problem and there is lack of both bed space and beds especially for under-fives.
A visit to Ward 5A, Weekend Nation found that 106 under-fives had been admitted in a room that had only 26 beds. There is an average of 120 admissions in children wards, where four children are now sharing a bed. The referral hospital was built for 800 beds.
KCH spokesperson Chiyanjano Kazombo said on Wednesday the congestion has worsened at the facility due to limited resources in terms of personnel and drug shortage.
She says, the hospital registers high numbers of malaria cases during the rainy season, but the number of nurses on duty does not change. It remains four, and at times even two per shift.
Said Kazombo: “As much as management of the hospital has prior knowledge of rising cases of malaria during this period, it is very difficult to prepare with limited resources that we have. How do we plan when the number of health personnel is the same and others are quitting.
“We are also still getting the same allocation for drugs and sometimes we are not supplied the drugs that we order from Central Medical Stores Trust [CMST] but rather what they [CMST] can supply at the time.”
Cashgate and the resulting withdrawal of budgetary support have contributed greatly to the challenges at KCH and the other three central hospital. Prior to 2014, donors would contribute towards staff training, recruitment and salary top-ups to attract and retain health professionals. But now, the ministry can no longer post intern doctors and clinicians to KCH due to lack of funding.
Mzuzu Central Hospital officials said to ease congestion, the facility no longer takes in-patients unless they are referrals.
Malawi fails to meet the World Health Organisation (WHO) minimum threshold of 23 doctors, nurses, and midwives per 10 000 population which is necessary to deliver essential maternal and child health services.
Effect of population boom
Ministry of Health Principal Secretary (PS) Dan Namarika said in an interview on Tuesday that population boom has also contributed to congestion of patients in public hospitals.
The PS said all the four referral hospitals were constructed when the country’s population, which is now estimated at 17.5 million, was below 9 million.
“Congestion in our hospitals is due to increased population against the existing structures. The central hospitals also act as primary and secondary health facilities [hence they take in more patients],” he explained.
Namarika said to reduce congestion, is looking into the feasibility of constructing district hospitals in Blantyre and Lilongwe.
“We have finished feasibility studies for both Blantyre and Lilongwe district hospitals,” he said. “Land for the construction of the two hospitals has also been identified. Construction of Blantyre District Hospital will start soon and will be followed by another in Lilongwe”.
Namalika said the ministry was also strengthening district visits by specialist health personnel to reduce referrals to central hospitals and improve capacity of staff at district facilities.
But Parliamentary Committee on Health chairperson Julian Lunguzi said government should take the blame for prioritising politically popular social projects such as stadiums over the weakening health sector.
“Our health sector is crumbling because of wrong priorities. All the [four] referral hospitals are old and cannot cope with the demands. Government should enforce primary health care. We should focus on setting up structures for primary and secondary health facilities to decrease traffic to central hospitals,” she said.—Additional reporting by Joseph Mwale, Mzuzu Bureau Supervisor.






We have Atupere as aminister for health.. Atupere useless man. 4billion is not enough. Now he can see that poor people are sleeping in corridors and no proper equipment or medicine.
All what I know cancer ku Europe ikugwira akuluakulu than young people. Malawi yugwila ana.
Some foreign companies and NGOs needs to banned in this country.. especially those in pesticide category.. those involved in Modified genetics crops.
MBS is not doing its job properly..
Above all ATUPELE is there as sign post. He’s not helping us…. the man is NON MEDICAL Kick him out
Children are being given katemera for medical trials in this country by Foreign NGOs.. ana akutenga matenda of which its hard sue these NGOs.. akubweretsa matenda womwe it will cost tax payers alot to cover what the government will borrow, these will continue giving burden to the tax payers( government) and also parents.. unless the government will put tough policy in it will not continue