Tackling chronic coughs
Every day, Chikumbutso Kufeyani from Chiwamba in Lilongwe has to feed her family. The rural woman, who sells doughnuts at Kanengo, leaves early for the industrial area.
The use of firewood to prepare food and doughnuts is part of her everyday tragedy. Her household is not connected to the national electricity grid even though distribution lines, installed as part of the country’s rural electrification programme, pass nearby.
She inhales huge amounts of smoke every day and she is haunted by frequent respiratory illnesses, says Kufeyani. So is her family, including her husband who burns charcoal. Plying her trade in the shadow of tobacco processing companies exposes her to narcotic fumes and other health hazards.
“Not all is bad,” Kufeyani says. “After all, I can afford cough lozenges and antibiotics when I notice signs of coughs.”
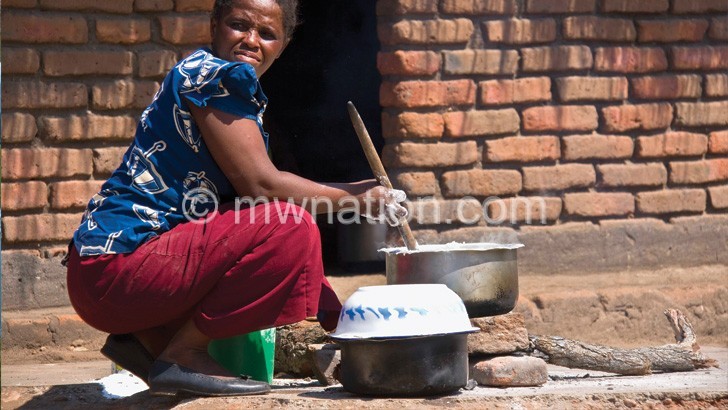
Chronic coughs are the reason thousands of Malawians seek health services
Medical experts say many people in the country are living dangerously-and this has to change.
Severe chronic airways disease and tuberculosis (TB), they say, reduce quality of life and livelihood for those affected.
Studies by the Ministry of Health show that coughs exert pressure on out-patient services amid numerous gaps in management of patients with respiratory symptoms.
“About 25 percent of those who access the country’s health facilities, mostly women and children, have symptoms of poor lung health,” deputy director for preventive health services Doreen Ali confirmed the reports.
This usually results from being exposed to smoke either in food preparation or when someone nearby is smoking, she explains.
Research for Equity and Community Health (Reach) blames exposure to smoke for sparking an increase in non-communicable diseases (NCDs) in Malawi and other countries south of the Sahara.
The non-communicable respiratory diseases include chronic airways disease which comprises asthma, chronic obstructive pulmonary disease and bronchiectasis.
Risk factors for these conditions include tobacco smoking, indoor air pollution from wood fuels and infections.
“Despite the burden of NCDs in Sub-Saharan countries, there does not seem to be much attention paid to address them. They still pose a big challenge in the region” says Reach executive director Hastings Banda.
He urges Malawians not to rush to buy drugs, but to seek assistance from qualified medical personnel.
Buying drugs from shops without proper prescription is detrimental and costly, he says.
Reach is conducting a cluster randomised trial to improve recognition, diagnosis and management of asthma, TB, chronic obstructive pulmonary diseases and other airflow conditions.
Researcher Kingsley Chikaphupha says: “We noted that delayed diagnosis and treatment initiation leads to severity of disease and complications like bronchiectasis and lung collapse arising from TB.”
These conditions threaten the lives and productivity of those affected, he warns.
“At worst, severe airflow limitation may lead to functional disability and high mortality,” Chikaphupha warns.
But the Kufeyanis personify the plight of millions of Malawians, with nearly 70 percent of the population living in rural areas.
In their remote settings often shunned by health workers, delayed diagnosis is common, health facilities are far apart.
Low access to electricity leaves many at risk of suffering respiratory illnesses, including TB
World Health Organisation (WHO) ranks TB as the world’s leading infectious cause of death in adults.
It kills almost 1.4 million out of the nearly eight million cases that occur every year.
Sadly, the current detection process is burdensome.
Professor Bertie Squire of the Liverpool School of Tropical Medicine, who are part of the Triage 2 Trials at Reach, says it is time to fully diagnose lung health defects.
“Sometimes, it requires the patient to visit the clinic for about eight times before a diagnosis is made,” the expert says.
But even in the urban centres, the shortage of medical staff still makes it difficult for respiratory challenges to get the time and attention they deserve.
Ali described it as unfortunate that most health facilities have become curative centres instead of preventive entities.
“The opposite would have served the country greatly in both social and economic terms,” says the Ministry of Health official.
According to Ali, the country needs to promote “a practical approach to lung health” by engaging informal healthcare providers on the detection and management of respiratory illness at primary health care level.
“Building capacity at primary health care level can significantly reduce the threat of respiratory illnesses in the country in the face of the booming population,” she says.
About 17 health surveillance assistants and patient attendants randomly picked from 12 health centres in Dowa and Ntchisi have since been trained in diagnosing TB and other chronic respiratory diseases right in their communities.
Squire put the training financed by Norway’s LHL International in context: “These community health workers will be helping out in terms of the detection of the conditions.
“Skilled medical workers will still be doing all the prescription and other curative duties.” n





