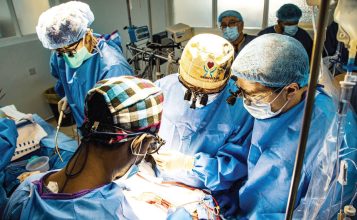
Taking HIV response beyond 90-90-90
Its 2020, the turning point in the global push to end the Aids pandemic. Although the country has surpassed 90-90-90 goals, declines in new infections remain too low. This is a call to renewed commitment towards HIV prevention, our features editor JAMES CHAVULA writes:

Recently, 90-90-90 has become the theme song of the global push to end new HIV infections. Both policymakers and change agents working to roll back the pandemic that once reduced Malawi to a nation in mourning—with coffin workshop lining all major streets—say it is the magical code towards ending the spread of the virus which causes Aids.
Policymakers and scientists envisaged all nations ending Aids by 2030 if they ensured that by 2020, at least 90 percent of people with HIV virus know their status; 90 percent of persons diagnosed with the virus start taking treatment without fail; and 90 percent of the population on treatment achieving suppressed viral load until it can neither be detected or spread.
Dr Dan Namarika, principal secretary for the Ministry of Health, is happy that Malawi has surpassed two 90s, thanks to life-changing responses which includes self-testing as well as the test-and -treat policy in which everyone who test HIV-positive is supposed to be put on treatment immediately.
“We have done extremely well in all areas. Currently, we are at 92-84-91, meaning that we have almost surpassed all 90s, except one. Beyond 2020, we need to aim for 95-95-95. This is achievable if we build on the successes we have registered largely because of the policies and HIV management systems government has put in place,” he says.
Dramatic change
Namarika was admittedly motivated to become a medical doctor by a huge burden of deaths caused by infections which thrive when HIV breaks down body defences.
Before the introduction of antiretroviral drugs in 2005, the opportunistic diseases, including tuberculosis (TB) and meningitis were claiming at least seven people every hour.
“People were dying like flies,” says Karen Msiska, spokesperson of National Aids Commission. “ARVs are credited with the reduction of Aids-related deaths from 64 191 when the programme took off to 12 978 by the end of 2018.”
Last week, Namarika looked back to the days of mourning when funerals were an everyday occurrence and coffin workshops were flourishing.
He says it is incredible people living with the virus can test themselves in the confines of their homes and access free treatment in both public and private health facilities, including those run by the Christian Health Association of Malawi (Cham).
He says: “The change is dramatic; it’s so tangible every household feels it. Once the BBC aired a documentary showing how coffin workshops in Mchesi Township [near Kamuzu Central Hospital] in Lilongwe are no longer cashing on Aids-related deaths, but furniture.
“And last year we saw a video clip, which went viral on the social media, showing a carpenter complaining that coffin business is not rewarding any more. That’s incredible.”
But the leader of the country’s healthcare workforce is worried that the country fell six-percent short of the target to ensure 90 in every 100 people diagnosed with the virus start taking the life-prolonging drugs instantly. This denies them a chance to not only live a healthy life but also reduce the viral load to undetectable levels.
He is also concerned that the dramatic drop in advanced HIV cases and deaths caused by Aids are breeding complacency leading to a rise in new infections, especially among adolescents and young people, “because they don’t experience HIV as it used to be”. To him, this is dialling back the epidemic at a time nearly 1.1 million people in the country are living with the virus.
“We need to restore the momentum to prevent a surge in new infections. Complacency may erode the gains we have achieved,” he says.
Although Malawi has scored 92-84-91 in the global race for 90-90-90, the pursuit of the silent 90—preventing new infections—could be falling behind in the national response.
Prevention still slow
In 2016, Malawi joined the global coalition on HIV prevention, committing to reducing new cases of HIV by 75 percent by 2020. This required the country to trim the number of new infections from 59 000 in 2010 to 11 000 in 2020.
Despite the promise to accelerate HIV prevention, declines in new infections remain too slow.
National figures endorsed by NAC show nearly 38 000 people countrywide acquired HIV in 2019—up from 36 000 in 2018.
In October, the Global HIV Prevention Coalition’ reported that Malawi is one of the countries falling short on HIV prevention targets despite targeted Global Fund investments.
The coalition convened by UNAids and UN Development Programme comprises over 40 member States, civil society organisations, highly at-risk population networks and international organisations such as the Global Fund.
Only two of the 26 reporting countries were “virtually on track” to achieve the 2020 target, the second progress report released three month ago.
“Definitely, we have missed the boat when it comes to the HIV prevention targets we made in 2016. Although we are making tremendous progress in terms of treatment, but not much is happening on the prevention side.
Locally, new infections have increased by almost 2 000 since 2018 instead of going down. Globally, the annual number of new infections has remained around 1.8 million for the past decade,” says Ulanda Mtamba, a former fellow of the Aids Vaccine Advocacy Coalition (Avac), which is affiliated to the Global HIV Prevention Coalition.
UNAids reports that the need for accelerated HIV prevention is particularly acute among women, who account for slightly over half of new adult infections. In Malawi, the pandemic has a woman’s face, with adolescent girls and young women being the worst hit and disproportionately at risk.
Mtamba wants the Ministry of Health to expand the preventive measures for women and other at-risk populations.
Women, especially adolescents, do not have the power and many options for safe sex. Despite the high new infection rates among women in the country and globally, women do not have enough HIV prevention in the toolbox. Currently, it is only a condom. Sadly, women don’t have much say on condom use,” she says.
The activist says no country can successfully bring down the figures without reaching at-risk populations with methods that work.
“For the nation, this is the best time to ask ourselves: Are we investing our time, energy and resources in the relevant sectors? Are we reaping the desired results?” she states.
Interestingly, Namarika says it time to invest more in prevention even though treatment gets a lion’s share of financial inflows propelling the country’s hugely donor-funded national HIV response.
He explains: “We may have not reached 11 000 by 2020, but the number of new infections has fallen dramatically from over 55 000.The main challenge with prevention is that change is not visible immediately.
“Unfortunately, donors are looking for quick gains. As such, treatment gets more funding because they need data demonstrating the impact of their investment. So we have to show impact in line with donors’ deadlines and budgets.”
Donors bankroll up to 85 percent of Malawi’s healthcare system, with national efforts to combat HIV and Aids equally starved of domestic funding. Just last month, the Global Fund announced a $513 million (an equivalent of K371 billion) for the fight against malaria, tuberculosis and Aids.
In November, Minister of Health Jaappi Mhango announced the new ambition to ramp up health financing to ensure it gets 15 percent of the national budget every year. Now, his ministry gets just about six percent of the K3 trillion budget.
However, Maziko Matemba, the board chairperson of Malawi Network for Aids Service Organisation (Manaso), says the successes in the fight against HIV and Aids will remain fragile unless government start honouring the Abuja Declaration of 2001 in which African nations committed to allocate at least 15 percent of the national budget towards improving healthcare provision.
He says: “Apart from respecting the Africa Union declaration, government should ensure that every sector contributes two percent of its funding towards tackling HIV and Aids. If we do this, we will reduce donor dependence.
Besides, let’s have a fair discussion on where we’re doing well and why we are failing in vital areas, like putting people on treatment and preventing new infections.”
Reducing HIV risk
Looking beyond the 90-90-90 global agenda, Namarika says there is need to increase the investment in efforts that place the thrust on averting HIV transmission.
“We need to find out what’s driving new infections, but we shouldn’t lose sight of the fact that the prevention side also informs the three 90s.
“If people get tested, those found negative take necessary measures not to get infected and those found positive immediately start treatment and achieve viral suppression to an extent that they cannot spread the virus.
Grace Kumwenda, from Pakachere Institute for Health and Development Communication, dials up the science that shows consistent use of ARVs actually eliminates the risk of HIV transmission, but wants more reliable methods in the country’s toolkit for HIV Prevention.
She told journalists in Blantyre: “ART helps people enjoy good health and live longer while preventing new infections, but we need more preventive measures, especially for women. A man has condoms and voluntary medical male circumcision, but a woman has none except the female condom few people use.
“Culturally, she cannot bargain for protected sex. If she does, she is seen as promiscuous. We need to expand preventive measures that put the power in her hands to enjoy safe sex.”